A Hope and A Future
November 19, 2021
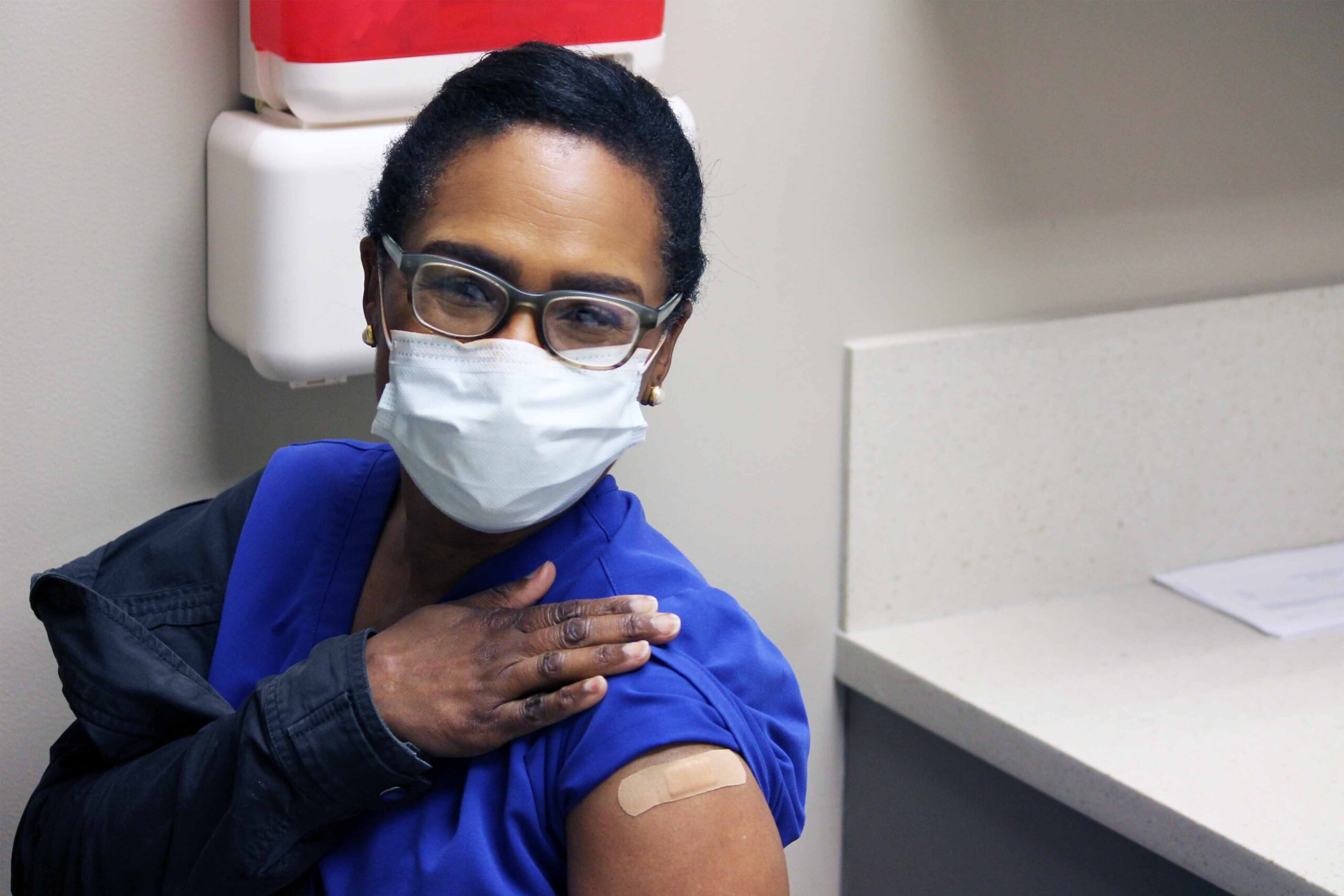
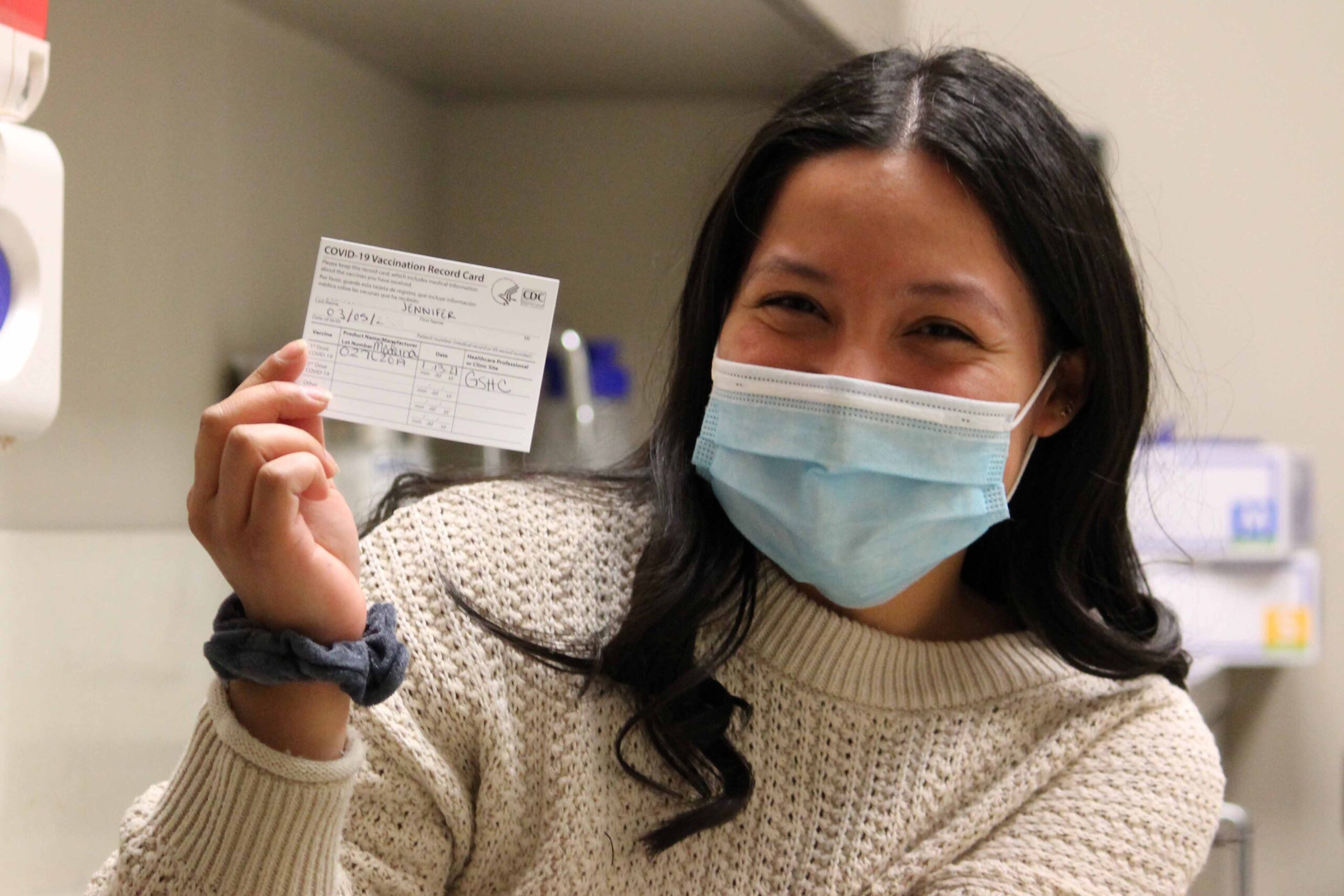
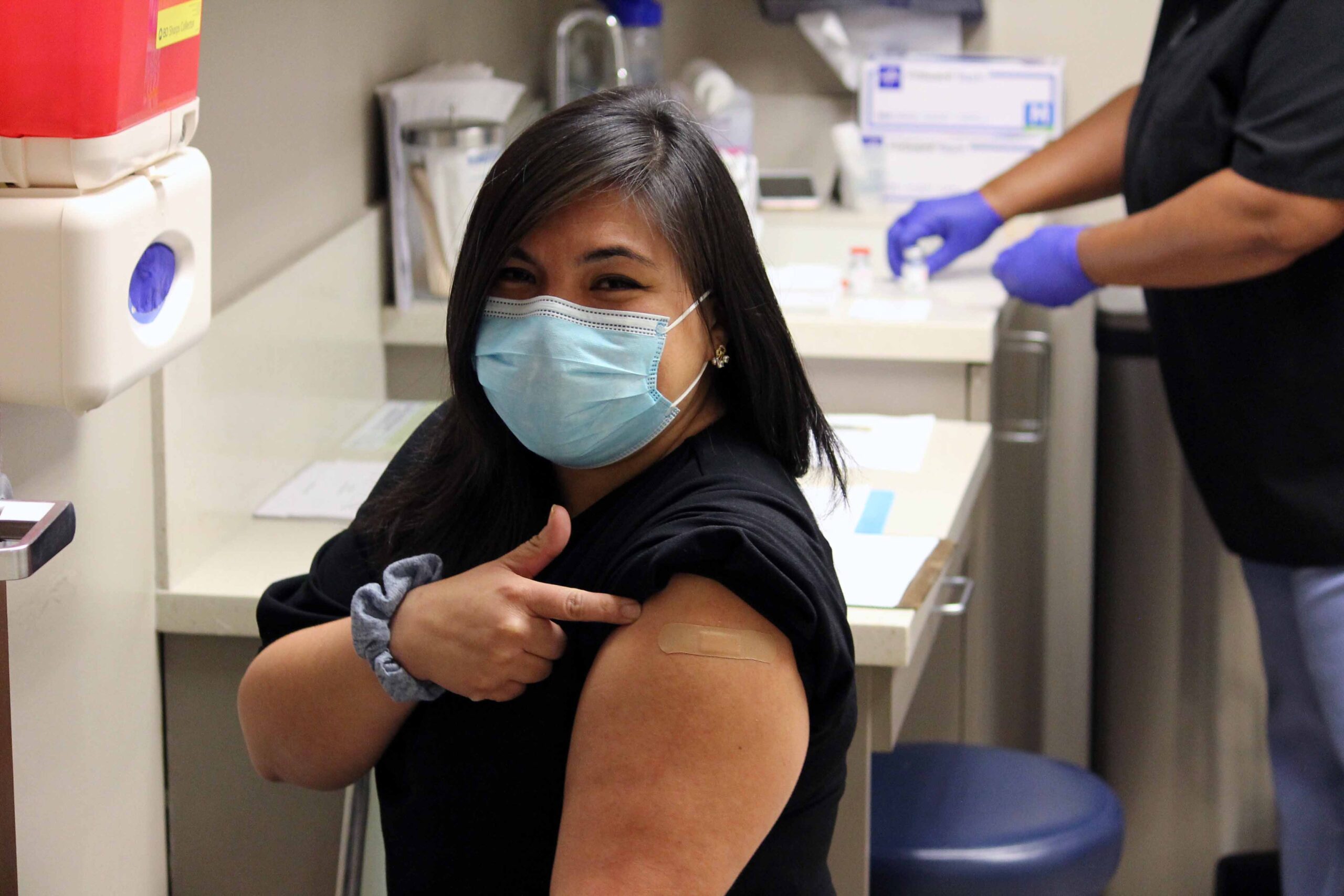
We are officially able to give the COVID-19 vaccine to our pediatric patients and the pediatric community at large!
On Saturday morning, two of my kids received Good Sam’s first doses of the Pfizer COVID-19 vaccine for kids ages 5 to 11. My boys got out of bed early and talked excitedly about the vaccine as we got ready to head to the clinic. Tre, our medical services coordinator and vaccine-giver extraordinaire, welcomed us to Good Sam and then she and I went through the checklist and procedures a couple times, making sure we were ready for our first day of administering pediatric doses. Tre had my kids laughing as she administered their vaccines; they hardly knew it happened. Then they proudly took a picture showing off their band-aids and gave permission for Good Sam to post it, so they could “help other kids know it’s okay!”
Since the beginning of the pandemic, my kids, their friends, and the kids we see at the clinic are vigilant mask wearers. They have never questioned why they had to wear masks. In fact, my 7-year-old completed an assignment for school entitled “Why I am a hero” and he wrote, “I am a hero because I wear a mask to keep other people safe.” Yet despite all our efforts, our kids tested positive for COVID-19 because I brought it home. They had already been in quarantine for a week when I ran their tests myself and watched each turn positive. I took a minute to get myself together before reassuring them that they would be okay, but that this meant another 10 days inside.
The feeling I had watching them get vaccinated reminded me of watching our staff get their first doses in January. Though my kids weren’t seeing sick patients and putting their own health at risk on a daily basis, they, like all the young people of their generation, made scarifies and had their worlds turned up-side-down during the pandemic. Without warning, their school moved to a virtual setting and for a year they spent their days learning via Zoom, without the consistency of friendships and social interaction that makes school enjoyable. Furthermore, because of my work, we enforced a strict quarantine on our kids, particularly until I was fully vaccinated. They missed out on playdates; we turned down birthday party invitations; many of their favorite seasonal activities were brought to a halt. They didn’t see their grandparents.
Today, I am so thankful for another way to protect my kids. I can’t describe the joy I felt watching kids come into the clinic to get vaccinated yesterday. But my kids and I also know that vaccination isn’t just about them. Kids aren’t the ones dying of COVID-19 but their vaccination rates move us closer to herd immunity in the community. They are getting vaccinated so they don’t spread COVID to their grandparents, or their teachers, or a classmate with a compromised immune system. COVID rates have fallen since the Delta surge this summer, but they are plateauing at far too high of a rate. Winter is coming and our health care system and workforce simply cannot sustain another surge. I see my boys and their peers getting vaccinated and I feel hopeful; but if I’m honest, I’m also apprehensive of possible future surges and stalling vaccine rates. I hope what we learn from our kids is that the choices we make to be safe and prioritize the needs of those around us, are the way out of this pandemic.

Breanna Lathrop, DNP, MPH, FNP-BC
Chief Operating Officer
Good Samaritan Health Center
Ways to Support Our Nation’s Recovery From COVID-19
July 20, 2021
COVID-19 testing centers are closing due to a lack of demand for testing. Vaccine appointments are readily available across the U.S. The nation is reopening, and masks are off. This season offers a moment to reflect and review the fallout of COVID-19. The newly published CDC report indicates that life expectancy declined by a year in the first half of 2020. Businesses and venues will reopen, and children will go back to school, but over 600,000 lives were lost forever from COVID-19. The impact of delayed care, limited access to healthcare, financial loss, and trauma/stress from COVID-19 will not be fully known for years to come.
This loss of life years is not distributed equally. The life expectancy gap between white Americans and people of color increased during the pandemic. In 2019, the average life expectancy gap between white and black Americans was 4.1, with white Americans living longer. By the end of the first half of 2020, this gap had increased to 6 years. Black men followed by Hispanic men experienced the most significant decline in life expectancy between 2019 and 2020. This report is another illustration of trends we have seen from the start of the pandemic. Communities of color and hourly, essential workers have born a disproportionate share of COVID-19s morbidity and mortality.
When we see the help wanted signs and read about the shortage of hourly workers, we need to remember that many left their jobs because they got sick. Some didn’t return because they died. Others decided that dying for a job that barely made a living wasn’t worth it; that being called an essential worker yet treated as dispensable didn’t compute.
So what do we do? We keep working. For Good Sam, this means continuing with COVID testing, care, education, and vaccination and providing high-quality, flexible, and compassionate care to people who are often left without it. While this has been our commitment since opening 22 years ago, we commit to listening and learning to better meet the needs of our community and patients in the ways that are most meaningful to them.
If you are looking for ways to support our nation’s recovery from COVID-19, I’ll offer a few suggestions. First, get vaccinated and share your vaccine story and encouragement to those that are still hesitant. Continue to consider the safety of others, particularly in indoor or group spaces. Although we are in a much better place than last summer, COVID-19 is not gone. Support the growth and sustainability of our public health sector. When we prioritize and fund public health and preventive care, we decrease health disparities. I am thankful that this June does not look like June 2020, but we have a long road to recovery ahead.

Breanna Lathrop, DNP, MPH, FNP-BC
Chief Operating Officer
Good Samaritan Health Center
We Can Listen, Learn, and We Can Empathize.
March 20, 2021
Atlanta again is the location of national tragedy. Discrimination and hate crimes against AAPI communities have increased with the pandemic. The pandemic has been tragic and exhausting for everyone, but for AAPI communities, this has been augmented by intensified racism and baseless blame. This week in Atlanta, eight people lost their lives, not to the pandemic but due to violence and hate.
The day before the murders of eight people, I was seeing one of my favorite, longtime patients. Over the years, she has shared with me pieces of her Chinese culture, from traditional healing practices to meals she prepares for me the night before her visit. She suffers from a rare neurological condition, and I remember years ago, she saw a specialist at a large medical center. She was given a medication that is often metabolized differently in people of Asian descent. She reacted severely to the medication, and the neurologist told her the symptoms she was having couldn’t be from the medication as she suspected. The dose she was on couldn’t be harmful; he had told her unless she was Asian. Her father was white, and she took her husband’s last name in marriage, meaning she didn’t fit the specialist’s idea of Asian. He had never asked, and she had no reason to question his medical judgment. Hearing her experience challenged me that racism not only hurts when it leads to violent crime. We each hold biases, including those of which we are not fully aware. But we are also all capable of change. We can listen, we can learn, and we can offer empathy.
To our AAPI brothers and sisters, including our patients, volunteers, and community of supporters, we grieve with you and stand in solidarity.

Breanna Lathrop, DNP, MPH, FNP-BC
Chief Operating Officer
Good Samaritan Health Center
31,906
March 9, 2021
Friday marked the anniversary of our COVID-19 helpline. One year ago, the world was shutting down, and we were rapidly innovating to respond to our patients and community. As of Friday, our helpline team of volunteers and staff have responded to 31,906 calls. There is perhaps nothing that summarizes this year as much as that number.
The early callers were mostly routed to providers. I remember talking to terrified individuals through their questions, thinking that I knew little more about COVID-19 than they did. There was no testing, no treatment, and little to do other than help patients decide whether they needed the emergency room. A few weeks later, we were able to schedule people meeting strict criteria to test through the department of public health and route others to the first sites set up by private companies.
As summer arrived, we launched our partnership with CVSHealth and brought rapid testing to Good Sam. The call volume exploded, and our team fielded hundreds of calls a day, booking out days in advance. Those calls represent so many sick people. Positively rates hit 50% regularly at the test center, and working tirage felt like a revolving door. The summer is forever clouded by the patients we lost and those we cried with as they lost loved ones to the virus.
In the fall, the volume fell to a more manageable pace along with the case rate in Georgia. The helpline rallied new volunteers, and we re-grouped. The helpline we thought was a temporary solution was going to be needed for the foreseeable future. We were ready when the numbers started to spike again. In some ways knowing what to expect made it easier, and in other ways, the thought of reliving the summer felt overwhelming. I wondered if we had it in us to weather another surge. We did.
Just as the winter surge started to decline, vaccine calls started. Today calls are a mix of ongoing testing requests and people calling to schedule vaccination. It feels hopeful, but I check the death count every day. We get calls from people who will be diagnosed for the first time and others who have contracted the virus a second time. We are managing the long-haul COVID patients with symptoms months after surviving the virus and responding to the consequences of delayed primary care. Hope is mixed with the reality that we will feel the pandemic's impact for a long time to come.
The 31,906 calls taken this year tell the story of the trauma of this pandemic and the goodness of humanity shown through this long and difficult year. Our volunteers have organized, trained, recruited, and responded in a way that equals nothing else I have seen in my entire career. I'm going to make sure we don't forget our systems' inequities that have been loudly on display throughout this pandemic and even in vaccination. But I'm also going to tell the story of the heroes who have given their time and energy to respond with love, care, and endurance.
To the thousands who called us: I am so sorry for how this pandemic has uprooted your life, for the pain and sickness you have experience. To the Helpline team, our volunteers, and partners: thank you for changing our little corner of this world.

Breanna Lathrop, DNP, MPH, FNP-BC
Chief Operating Officer
Good Samaritan Health Center
We Won't Stop Trying!
February 14, 2021
This week our staff and volunteers received the second dose of the COVID-19 vaccine. This also marks the end of our first month as a Department of Public Health vaccine site. I am thankful and tired. Fatigue is a common immune response symptom after the vaccine, but it's more than that. Becoming a vaccine site has meant new processes, training staff and volunteers, reading lengthy vaccine updates every other day, monitoring vaccine temps and timing when each vial leaves the freezer, and responding to people's questions, concerns, and needs seeking vaccination. Our supply allows us to provide about 100 vaccines each week. Sometimes it feels like a small win for the months of waiting for and massive effort behind vaccination.
But it is absolutely worth it.
While case rates have dropped over the past few weeks, the pandemic wages on. One man I saw this week was on his fifth day of fever and diarrhea with COVID-19, but his breathing was fine so there was little I could offer. That same day, I explained to a mom that she and all of her children just tested positive. The patient I sent to the ER two weeks ago with low oxygen levels hasn't returned my calls to check on her. Experience tells me this is not a good sign.
One hundred vaccines a week seems very small against the raging pandemic.
Our work at the clinic can often feel small against our patients' health disparities and the inequities in our health care system. Last week, I spoke with NPR on a national story they were publishing about the lack of vaccination sites located in areas made up of predominantly communities of color. Today, during our homeless outreach clinic, I was always reminded of how people's bodies bear the stress of persistent inequity.
Yet change is born of consistent, committed efforts. It is the result of resiliency and a refusal to accept the current reality as the only option. Change happens when we commit to doing all we can now, even if our offering is small. Each vaccine, each mask worn, each quarantine followed is a step toward controlling the pandemic, just as each patient who finds respect, compassion, and accessible health care through our doors is a step toward collective healing.
So even if only ten dosages of vaccine show up this week, we will vaccinate ten people. We may not have the ability to end the pandemic or eliminate health disparities, but it's not going to stop us from trying.

Breanna Lathrop, DNP, MPH, FNP-BC
Chief Operating Officer
Good Samaritan Health Center
A Good Day
January 13, 2021
Today is a good day. At 8:30 am this morning, we started the two-day process of vaccinating our staff, our volunteers, and our interns. For ten months now, I have watched my colleagues grapple with the realities of managing COVID-19 at the clinic.
Our COVID helpline has responded to 26,075 calls.
Our team has directly provided 980 COVID tests and consultations for people with COVID-19.
In partnership with CVS, we have helped test 20,597 people at the rapid testing site.
We watched and cheered and took pictures as the first employee vaccinations took place. In our triage area, next to our vaccination room, I put on my N95 and my PPE to start testing children. The first child tested positive. So did two of the next three. I watched employees walk in and out from getting vaccinated while I walked back and forth from triage, testing kids, and discussing positive results with parents. It was a surreal mix of hope alongside the genuine persistence of the COVID-19 pandemic.
Thank you to our staff and volunteers for the months of service you have given Good Sam and our patients. A vaccine will not erase the hours of extra work, the pain of what you have seen and experienced, or the ongoing challenge the pandemic will bring us in the months to come. But it is a bit of hope. Today, you go home with more than just a mask. You go home with the start of protective immunity and a vision for better days to come. You deserve this, and I am so thrilled to watch you receive it.

Breanna Lathrop, DNP, MPH, FNP-BC
Chief Operating Officer
Good Samaritan Health Center